Cervical Cancer: A Preventable and Treatable Tumor
Cervical cancer is one of the most common malignant tumors among women, with an incidence rate ranging from 73% to 93%. It ranks as the fourth most common cancer in women worldwide, though its incidence and mortality rates vary significantly across regions and countries of different income levels. In recent years, there has also been a noticeable trend of younger onset.
According to the World Health Organization (WHO), in 2022 there were approximately 660,000 new cases of cervical cancer globally, and about 350,000 women died from the disease. Over 94% of these deaths were attributed to inadequate screening. The cure rate for early-stage cervical cancer exceeds 90%; however, in many low-income countries, due to shortages of radiotherapy equipment and poor medical infrastructure, only about 30% of patients receive standard treatment. On an individual level, timely HPV vaccination and regular screening remain the most effective means of prevention.

Treatment of Cervical Cancer
At Foshan Fosun Chancheng Hospital, cervical cancer treatment follows international standards and is tailored according to the cancer stage and the patient's overall health. The main treatment approaches include:
1. Minimally Invasive Surgery
• Suitable for early-stage cervical cancer (Stage I–IIA). Common surgical procedures include:
Cervical conization (recommended for women who wish to preserve fertility), Total hysterectomy, Radical hysterectomy with pelvic lymph node dissection. The goal of surgery is to completely remove the cancerous tissue.
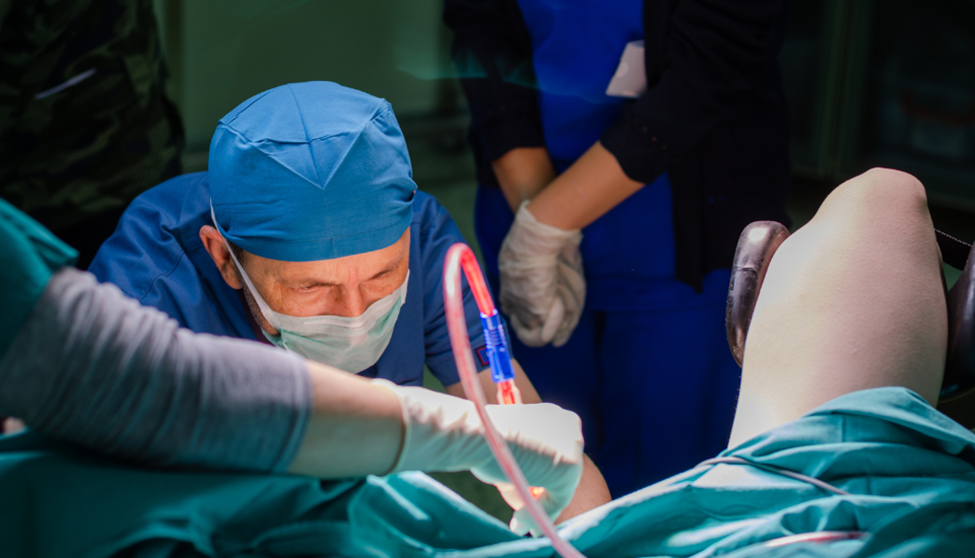
2. Radiation Therapy
• Includes external beam radiation therapy (EBRT)—which uses a linear accelerator to precisely target pelvic lesions—and brachytherapy (internal radiation therapy)—which delivers radiation directly to the tumor site to enhance local efficacy.
This method is suitable for patients in middle to advanced stages, those with postoperative residual lesions, or those at high risk of recurrence. Radiation can be used alone or combined with other treatments.
The CyberKnife system represents one of the world’s most advanced treatment options for cervical cancer. It is particularly suitable for patients who are not good surgical candidates due to poor health or multiple comorbidities. This non-invasive treatment delivers highly focused radiation to control tumor progression and inhibit cancer cell growth without the need for surgery. Moreover, the rapid dose fall-off of CyberKnife ensures that surrounding healthy tissues are well protected.
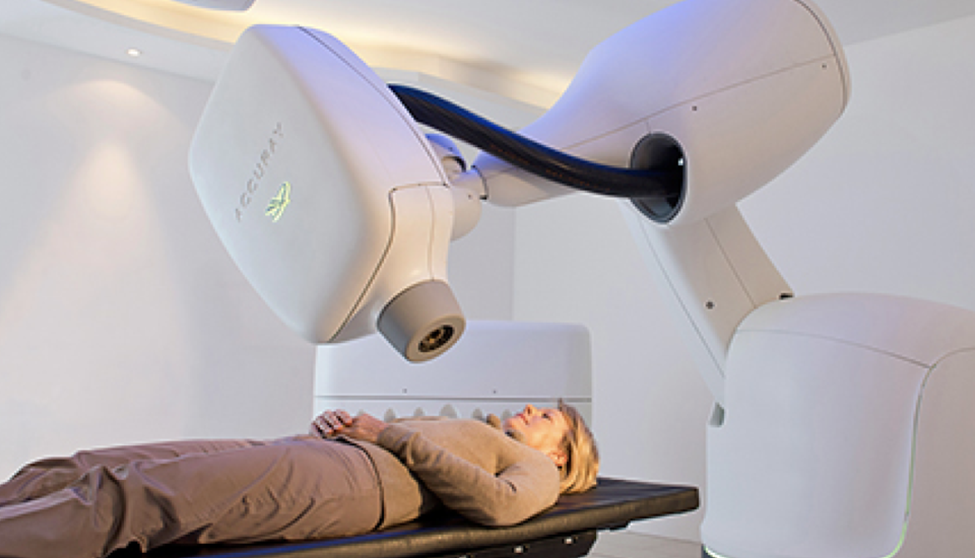
CyberKnife has been shown to effectively control local tumor growth and can also be used in combination with chemotherapy or other treatments.
Key advantages of CyberKnife (non-invasive radiosurgery):
1. Precision: Minimizes radiation exposure to healthy tissues, greatly reducing side effects.
2. Shorter treatment duration: Requires fewer sessions than traditional radiotherapy.
3. Quick recovery: Most patients can resume normal activities shortly after treatment.
3. Chemotherapy
• Commonly used drugs include cisplatin, carboplatin, and paclitaxel. Chemotherapy may be applied as:
Neoadjuvant chemotherapy (before surgery to shrink the tumor)
Adjuvant chemotherapy (after surgery to eliminate microscopic metastases)
Palliative chemotherapy (for advanced cases to relieve symptoms and extend survival)
Combination regimens are often preferred for better outcomes.
4. Targeted Therapy and Immunotherapy
• Targeted therapy: Focuses on specific molecular targets of cancer cells (e.g., vascular endothelial growth factor). Drugs such as bevacizumab are commonly used, often in combination with chemotherapy to enhance the efficacy in advanced cases.
• Immunotherapy: Activates the body's immune system to attack cancer cells. This treatment is suitable for some patients with advanced or recurrent cervical cancer and offers a new option for those unresponsive to traditional therapies.
5. Comprehensive Treatment
• For patients with intermediate or advanced disease, concurrent chemoradiotherapy or surgery followed by adjuvant chemoradiotherapy is often recommended to maximize the cure rate and minimize the risk of recurrence.
The specific treatment plan should be determined after evaluation by a specialist in gynecologic oncology, taking into account the pathology report and imaging results.
Regular follow-up is essential to monitor treatment outcomes and manage potential side effects.
It is strongly recommended to work with a medical team that communicates effectively with you, ensuring that you can confidently seek advice or a second opinion whenever needed.
Patient Story
01: Da Vinci Robotic Minimally Invasive Surgery for a 64-Year-Old Patient With Early Cervical Cancer
Ms. Ye, 64, tested positive for HPV16 during screening and was later diagnosed with cervical glandular carcinoma through biopsy. She traveled from Macau to the hospital for treatment, where Dr. Huang Hao, Director of the Gynecology Center, performed an innovative QM-C1 nerve-sparing radical hysterectomy using the Da Vinci surgical robot.
The day after surgery, Ms. Ye was able to get out of bed and walk. Only four tiny incisions were left on her abdomen, all healing well. After one week of observation, she was discharged.
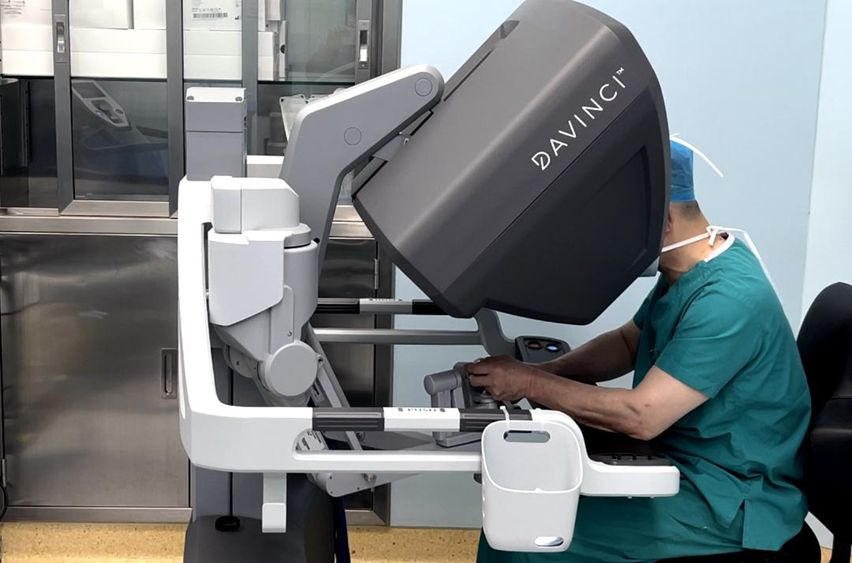
02: Multidisciplinary Removal of a Giant Cervical Canal Tumor in a 54-Year-Old Patient
Ms. Chen had previously undergone a subtotal hysterectomy. Years later, she mistook her growing abdominal bulge for weight gain until shortness of breath prompted medical attention. Examinations revealed a 25-cm giant cervical canal tumor that was tightly adhered to the intestines, ureters, and other structures, with dense vascularization.
The hospital adopted a two-step approach: "vascular intervention first, precise surgical removal second". The vascular surgery team first injected embolic agents, blocking 90% of the tumor's feeding vessels. Then the gynecology team performed a meticulous 3-hour surgery to remove the tumor, with only 100 mL of blood loss. The patient recovered well and was discharged successfully.
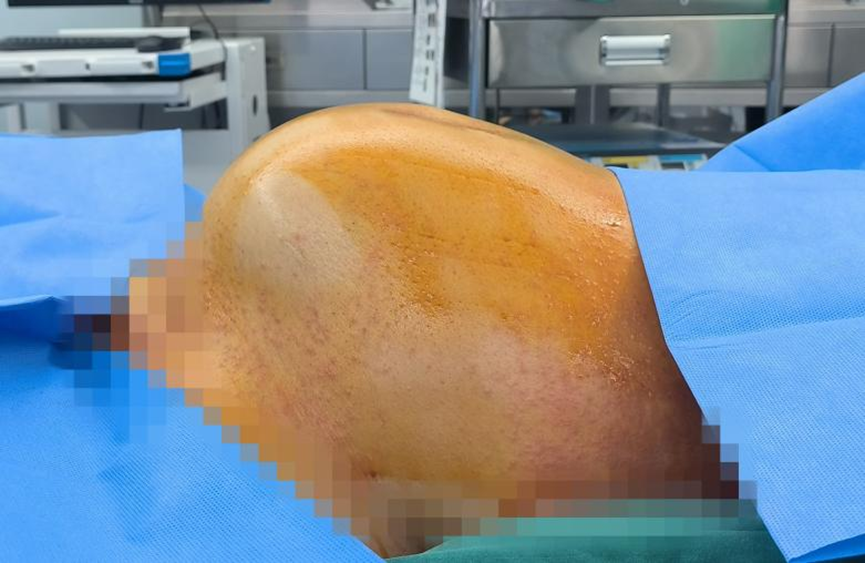
03: Precision Radiotherapy Combined With Interventional Treatment for a 79-Year-Old Cervical Cancer Patient
The patient, aged 79, presented with vaginal bleeding and abnormal discharge. At diagnosis, her cervical tumor measured 6×8×7 cm, and she declined both surgery and chemotherapy. The hospital administered precision radiotherapy, with CyberKnife accurately targeting the tumor while sparing surrounding healthy tissue.
After two months, the tumor had shrunk by half. Interventional therapy was then used to deliver medication locally and embolize the tumor's blood supply. Ultimately, the patient's bloody discharge completely disappeared, and her overall condition improved significantly.
If you would like to learn more about diagnosis and treatment options about Cervical Cancer, schedule a consultation with a specialist, or seek professional medical assistance, please don't hesitate to contact us anytime.
Md Mostofa kamal Phone: +8801817833123
Mr. Monirul Islam Phone: +8801914575388

